Dr. Millard’s Innovations in LipoSculpting & Fat Grafting Utilizing VASER Technology
Offered at our convenient location in Denver
The science of VASER was a quantum leap in liposuction, liposculpting and fat grafting technology. It was the first device that took into account and respected those tissues that surround the patients’ fat cells.
The Science of VASER “Selectivity”
Functionally there are three layers of fat that can be removed during the liposculpting process.
First, from the sub-dermis, immediately underneath the skin. Fat removal from this area with retention of the connective tissue releases the skin for maximal skin tightening and shrinkage. Removal of fat from this area is required if one is going to obtain significant skin tightening during liposuction/liposculpture.
The next layer down is the superficial fat compartment, which can be both reduced during liposuction for more dramatic size reduction, and/or shaped for 3-D and 4-D liposculpting. Again, preservation of the connective tissue and small lymphatics and blood vessels helps minimize tissue trauma while achieving maximal fat removal, along with further skin tightening by vertical contraction of the retained connective tissue.
The last layer is the deep layer which also has the same connective tissue, blood vessel, and lymphatic structures. Left relatively untouched while removing fat, minimizing this layer allows for further vertical skin tightening. Many post-liposuction irregularities and deformities are caused not by uneven fat removal, but uneven connective tissue removal. This is commonly seen with traditional suction-assisted liposuction which rips the fat and connective tissue, lymphatics, and small blood vessels. This means the tissue will be pulled harder down towards the muscle in areas where connective tissue remains and less contracted towards the skin where the connective tissue has been ripped away.
Therefore, one could have an “even” fat removal and an “uneven” connective tissue removal and still heal with deformities and irregularities. The VASER and the special “Atraumatic Cannulas” designed by Dr. Millard significantly reduce this risk.
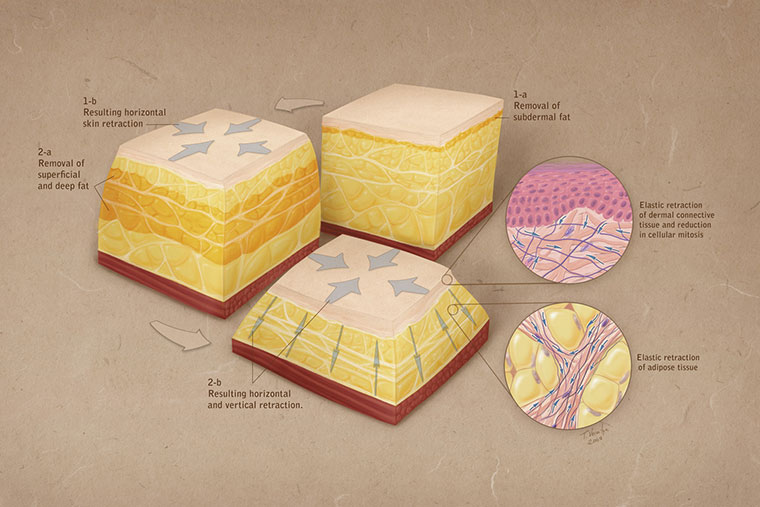
This is an illustration that describes the three functional fat layers that most body parts have over their respective muscle areas. The top most functional area is the sub-dermal Fat Layer. Its removal “unloads” skin from the fat to which it is glued, thus allowing the most significant amount of skin contraction seen as part of the three areas of fat removal. Ungluing the fat from the skin allows the skin’s own elastic properties to kick in and cause the skin to shrink.
In addition, the connective tissue still attached to the skin causes vertical tightening and shrinkage as well. Removal of fat in the next layer, the superficial fat layer allows for more dramatic change is size during liposuction and for shaping of the fat in this layer to conform with the patient’s own individual musculoskeletal anatomy during VASER HI Def (3-D) and 4D VASER Hi Def.
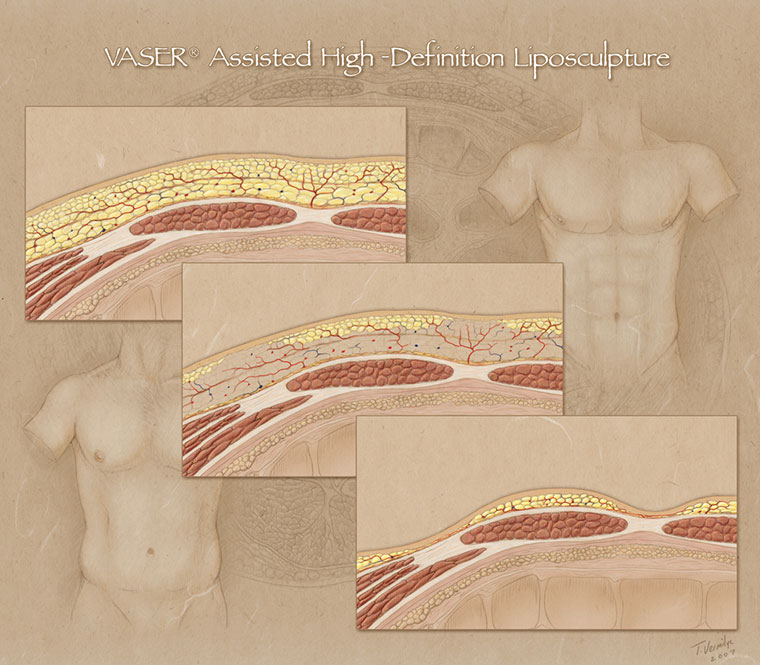
A three-layer process of liposuction/liposculpture is what makes VASER Hi Def sculpting possible. This is compared to the one-layer process of most traditional surgeon’s liposuction techniques.
The Three-Step Process of VASER Hi Def Liposculpture
- Step 1: Subdermal Fat Removal
- Step 2: Deep Fat Compartment Fat Removal
- Step 3: Partial removal of the Superficial Fat Compartment Fat & Shaping of the “Retained” Superficial Fat
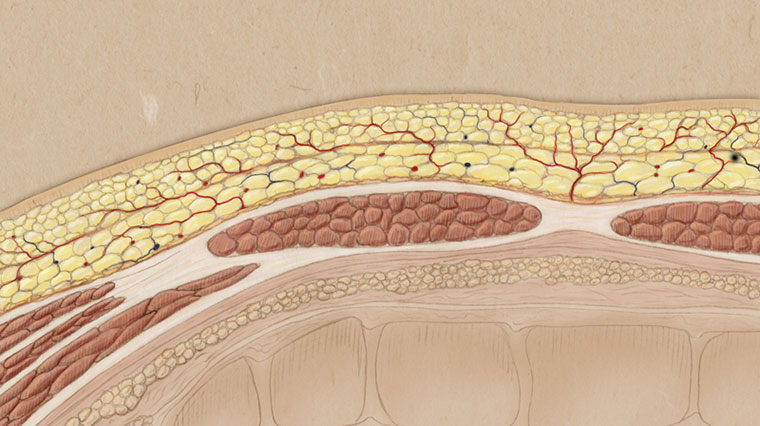
This image represents the two anatomic layers of fat overlying the rectus muscle. Remember the superficial fat layer is two “functional” Layers of Fat. The subdermal fat layer and the remaining superficial fat layer. Both of these functional layers sit on top of a membrane called the “superficial fascia” which separates these two functional layers from the second anatomical or third functional layer which is the deep fat.
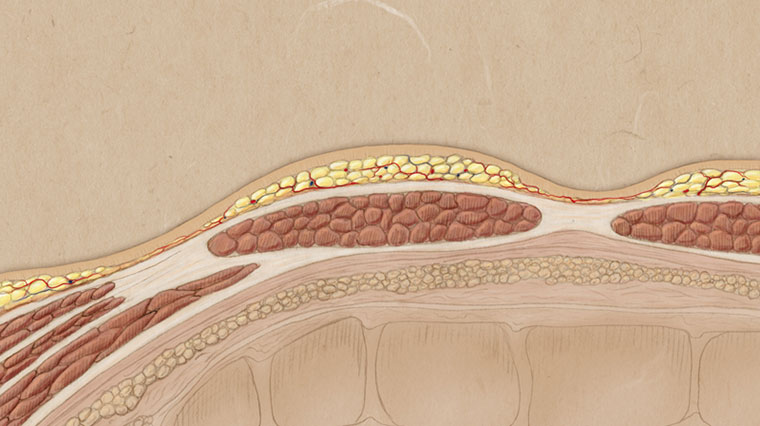
In this photo, the subdermal fat has been removed, the deep fat has been removed, and part of the superficial fat has been removed, with the remaining superficial fat shaped to augment the shape of the rectus muscle underneath.
In this photo, thanks to the retained connective tissue, complements of the VASER process and the atraumatic cannulas that were used to extract the emulsified fat, the skin can both tighten and also shrink wrap around the shape created over the patients rectus muscle, which has been used as a guide for sculpting the fat over it. The definition between the rectus muscles and the adjacent oblique muscles is made possible by complete fat removal of the three functional (two anatomical) fat layers and the retraction and tightening of the skin because of the VASER’s and the Atraumatic cannula’s ability to preserve the connective tissue that pulls the skin vertically down to define these muscle group. This represents two concepts.
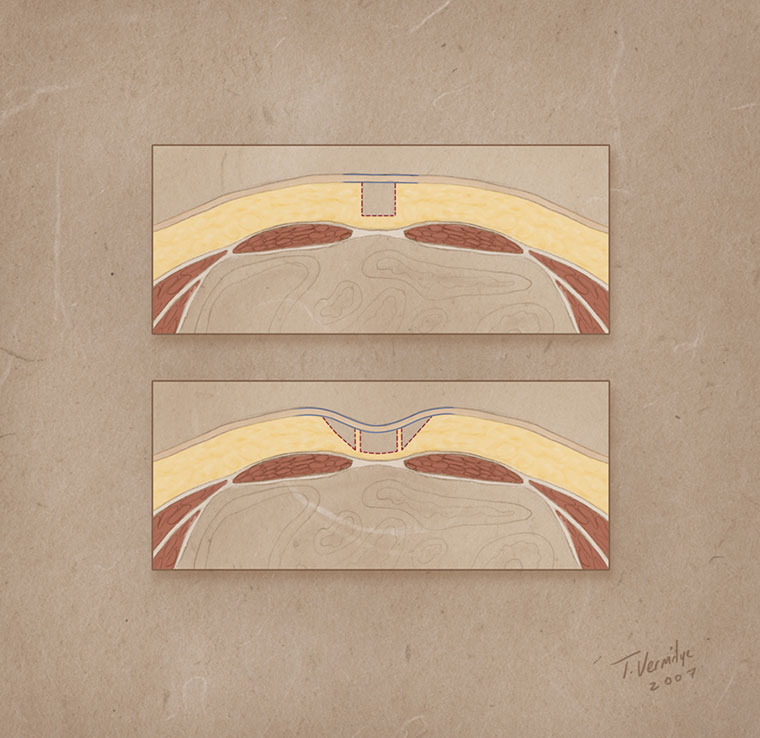
- The top is an example of both fat and connective tissue removal, commonly seen when doing “Traditional” liposuction (SAL). The space has been created to enhance definition, but there is no retained connective tissue, as it has been ripped out along with the fat. Therefore the skin fails to be pulled into the space created between the muscle groups.
- The bottom image is an example of what one would see when fat has been removed from the same space with the VASER and Dr. Millard’s Atraumatic cannula’s. Connective tissue has been preserved even though fat has been removed from the space. The skin can then be pulled into that space, thus enhancing of the definition between the muscle groups. This is a fundamental concept of VASER Hi Def and 4D VASER Hi Def Liposculpture.
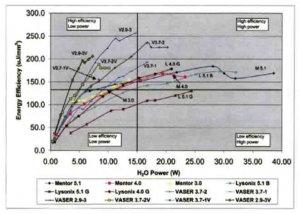
This graph demonstrates how the VASER was able to increase or improve on the efficiency of ultrasound for liposuction/liposculpture. The more the line is pushed to the left in the graph, the less total energy delivered to the tissues. The higher the points on the line are in the graph the more fat is being emulsified or separated from surrounding tissues. It is Dr. Millard’s belief that the combination of taut tumescence, emulsification, compression coupling, and the VASER Five-Ringed Probe push this curve both further to the left and higher in the points height on the curve, Said simply, more efficiency of freeing up of fat, faster, with less total ultrasound energy.
- Step 1: Subdermal Fat Removal
- Step 2: Deep Fat Layer Fat Removal
- Step 3: Partial Superficial Fat Layer Fat Removal & Superficial Fat Layer Reshaping
- Step 4: Intra Muscular Fat Grafting
- Step 5: Subdermal fat Grafting

The original probe design was a revolutionary change from the sharp edged energy that came out of the tip of the probe. The probes expanded the energy so that depending how many rings there were, more energy came out the side-rings, therefore, increasing efficiency of the ultrasound fat emulsification process. At the time, the three ring design was the maximal number of rings and approximately 50% of the energy came out the sides and approximately 50% of the energy came out of the tip of the probe. The belief was that tip-energy was needed to get the probe into the fat so that the side-ring energy could do its work to disrupt or free the fat from the surrounding connective tissue, blood vessels and lymphatics. Approximately eight years into using the originally designed probes, Dr. Millard came to realize that efficiency of the VASER process could be improved. The culmination of this development process resulted in a “Five-Ringed Probe.”
The “Five-Ringed Probe” came about after much work by Dr. Millard to help increase the efficiency of the VASER process. One of the complaints of the VASER by many physicians was that it took too much time, that it took longer than traditional liposuction (SAL). The argument that was made by the folks at VASER was that even though surgery took longer, the outcomes were better for the patient. For many surgeons this was not enough to invest in this technology. This all changed with three key developments by Dr. Millard.
- Development of “Taut Tumescence”
- Development of “Compression Coupling”
- Development of the “5-Ring VASER Probe”
What resulted from these three developments was the following: A reduction of VASER time by 50-75% for a given body part — There is a direct relationship to VASER “dwell” time, meaning the time a surgeon runs the VASER in a patient’s tissues and the amount of surrounding tissue damage, pain, bleeding, etc. Reducing the time one runs the VASER in the tissues, reduces all of these variables. A reduction in the amount of time it takes to remove the “emulsified” fat after the first VASER step. In a majority of cases the time for this step has been reduced by 50-75%.
It seems the combination of taut tumescence, compression coupling, and the 5-Ring VASER probes, frees or separates the fat from the surrounding connective tissues, blood vessels and lymphatics more effectively than with older VASER methods using the one-, two-, or three-ring probes. This separation or “Emulsification” process is more effective even with VASER times that are much less than with the older VASER methods. The fact that the fat removal time has been reduced means less passes with the fat removal cannulas, again, resulting in less surrounding fat and tissue trauma.
Ultimately, for the patient, this results in less pain, bleeding, bruising and recovery time, with less surrounding tissue damage, which also results in less problems with deformities and irregularities as well. The combination of Taut Tumescence, Compression Coupling, and the 5-ring VASER Probe has resulted in VASER being the fastest liposuction/liposculpting technology on the market today. This is a benefit to both liposculpting surgeons and their patients.
Patients often ask how VASER works. Understanding how the VASER works might also help patients and surgeons understand how Taut Tumescence, Compression Coupling, and the 5-ring VASER Probe work so efficiently as well.
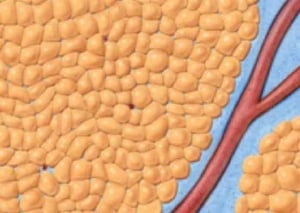
This image shows fat globules/cells all bunched up around a blood vessel, before any tumescent fluid has been injected into the tissues. All liposuction/liposculpting techniques start with injection of “Tumescent” fluid. This fluid does three things for traditional liposuction (SAL). It delivers epinephrine (or adrenaline) to the tissues which then acts on the blood vessels making them constrict (makes smaller), which makes the walls of the blood vessels thicker, and this makes them more resistant to tearing during the liposuction process. It delivers Lidocaine, which makes the process less painful for the awake patient, and helps reduce the pain after the surgery, whether the patient had the procedure awake or asleep with anesthesia. With VASER-Assisted Liposuction/Liposculpture, the Tumescent Fluid does a third and important step. The tumescent fluid itself is acted upon by the ultrasound waves delivered by the VASER probes. This is how the third step works: Tumescent Fluid is injected into the fatty tissues. Tumescent Fluid can only get into spaces that are larger than 5 microns (A very small unit of measurement used in human biology to explain very small distances and spaces).
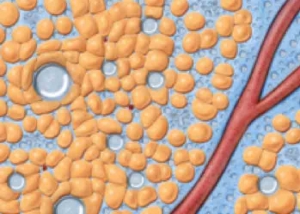
The only spaces or distances that are larger than 5 microns in the fatty tissues are the spaces fat cells have between fat cells, fat globules have between fat globules, and the spaces fat have between the surrounding connective tissues, blood vessels and lymphatics. All other tissues have spaces smaller than 5 microns and therefore Tumescent fluid can not get in between them. This is very important, because the energy delivered by the VASER probes has been set or tuned to work on the Tumescent fluid.
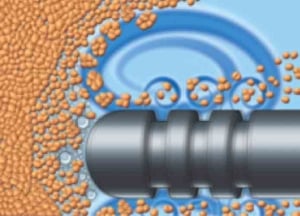
The VASER-Probe delivers energy to the tumescent fluid, and causes the “Gas Bubbles” within the fluid to expand and contract, causing the fluid molecules to continually get larger and eventually rupture. The rupturing of the fluid molecules causes the fat to separate from its surrounding connective tissue, blood vessels, and lymphatics, as well as causing the fat to separate from other fat. This results in a “Freed up” or “Emulsified” bunch of fat that is essentially ready to be removed with minimal amount of work.

There is one additional step that occurs with the VASER-Ringed probes, referred to as “Acoustic Streaming,” which is where the larger already freed up fat globules get processed to even smaller fat globules making them even easier to remove. The 5-Ring probe provides more surface area for both the emulsification step to work and for the acoustic streaming step to work. This makes the entire process more efficient, with less total energy required and less total time required to complete the process.

This is a picture of the older, less efficient fat extraction cannulas that were used and many still use today. They were a first real improvement in fat extraction technology. Dr. Cimino, the inventor of VASER, who also holds a doctorate in physics, spent four years working through many different designs to improve “Cannula Technology.” The result was the VentX cannula technology.
The VentX cannula incorporates the following: Aspiration Hole Size optimized to the diameter of the cannula. meaning large enough holes to remove fat, but small enough to minimize tissue damage. Aspiration Hole Separation is optimized to minimize tissue damage. Number of holes reduced from previous cannula designs. It turns out beyond a certain “Surface-Area” of holes, speed of fat removal is not improved, but increased surface-area of holes does increase tissue damage VentX technology — allows for a small amount of air to leak during fat removal, which minimized “Turbulence” and this decreased both fat damage and surrounding connective tissue, blood vessel, and lymphatic damage.
The Science of Millard Cannula “Selectivity”
- The VASER & Specialized Fat Removal Tools — Select for Fat; leaving the important connective tissue, lymphatics and blood vessels relatively untouched.
- It is helpful to remember that there is a complex set of tissues that surround fat and these tissues are very important to tissue health, even after the fat has been removed. Any design in any one of the steps that are part of fat removal, that can improve on, or minimize damage to these surrounding tissues, should be an important design addition to a liposuction/liposculpting surgeons arsenal of tools.

The Millard Cannula Design takes the VentX cannula (fat extraction) designs even further. Inspired by the fact that the combination of taut tumescence, compression coupling, and the five-ring VASER probes ability to more effectively free up fat from the surrounding connective tissues, blood vessels and lymphatics, Dr. Millard was inspired to design a cannula or fat extraction device that went even further to protect these all important surrounding tissues. The result was a “Beveled” hole design that did just that. The beveling process puts a space between the surrounding tissues and the edge of the hole during the fat extraction process. The slope of the beveling into the hole both slows down any tissues attempting to progress towards the whole as well as prevents the “Suction-cup” effect that traditional cannula hole designs have on fat and its surrounding tissues. In fact, these same beveled hole designs have been incorporated into his fat grafting cannulas as well for the same reasons, such as less trauma to fat as it is injected into surrounding tissues. Clinically, Dr. Millard has seen significant reductions in bleeding. bruising, and pain postoperatively in a majority of his patients. He has also seen a larger amount of intact transplantable fat to be used for fat grafting as a result of using these cannulas to harvest a patient’s fat for fat grafting.
Dr. Millard’s innovation didn’t stop with the liposuction/liposculpting steps. His next improvements were in the area of fat grafting. He is one of the first if not the first plastic surgeon to use real time Ultrasound Images to guide his fat grafting. It is a technique he calls Ultrasound-Image Guided Fat Augmentation Technique (UIGFAT). He designed special cannula technology that helps the cannula to be more visible during the fat grafting process. These cannula called “Echogenic” cannula incorporate two designs, one “Squire edges” and “Divots” like one would see in a golf ball. Both of these designs improve reflection of the ultrasound signal resulting in better visibility of where the cannula is when a surgeon is injecting fat. He strongly believes in this technique for the following reasons; Increased safety in that a surgeon can see blood vessels in the areas of fat grafting and stay away from them, thus, reducing the risk of a fatal fat embolism during fat grafting. More accurate placement of fat into whatever area a doctor wants to inject fat. Surgeons can see the difference between muscle and fat and also see the difference between the two anatomic areas of fat, which when fat grafted cause different results. Reduction of putting too much fat in one area causing increased risk of fat cysts and also failure of grafting in that area. An ability to put more fat in effectively, because a surgeon can see where he or she has placed fat and where they have not placed fat. In conclusion, Dr. Millard believes the older traditional method of fat grafting, blindly, or as he calls it Fat grafting by Brail, is an inferior method to being able to actually visualize where a patient’s fat is being grafted.



The Power-X Technology was designed for “Power-Assisted” fat extraction/aspiration of fat. It incorporates a rotational mechanism to the cannulas, that were in theory, to improve fat aspiration efficacy. Dr. Millard doesn’t use the Power-X technology for this, believing it to be unnecessary. The Power-X, though, in his opinion is an ingenious technology for a different reason. In his ever ongoing quest to make each step of the liposculpting process better and safer, he came to realize that the rotational mechanism could have great advantages in fat grafting. To accomplish this Dr. Millard designed cannulas that can be used to better integrate or mix the fat into its tissues once placed there.
The Millard “Fat Integrator” cannulas are designed to mix fat into tissues more evenly, once they have already been placed using his UIGFAT technique. It is akin to mixing chocolate chips into cookie batter more evenly. There is one additional advantage Dr. Millard came to realize using these cannulas and the Power-X. He can place, or graft, on average, an additional 50% more fat than he was able to previously using older fat grafting methods. He attributes this to two reasons: (1) More even placement of fat, and (2) Removal of surrounding water (Tumescent Fluid) during the integration process, resulting in more space for additional fat. Ultimately he is seeing an ability to create larger breasts than previously able to, using older fat grafting techniques. This also extends into area such as the male chest and male and female buttock augmentation as well.